Welcome to my last vlog, it has been fun sharing everything with you guys! Wrapping up strong with some electronic music by Ali Berger.
What is Rheumatoid Arthritis (RA) ?
Rheumatoid Arthritis (RA) is a chronic systemic autoimmune disorder primarily affecting joint linings. It is characterized by progressive cartilage destruction, bone erosion, and permanent joint deformity if left untreated. Studies consistently show that women are significantly more susceptible to RA than men, often developing the condition during their middle adult years. Genetic susceptibility alsp plays a substantial role in this disease, particularly involving the human leukocyte antigen (HLA) region. Environmental factors further elevate this risk, with cigarette smoking being a huge contributor to the development of disease. The hallmark clinical presentation of RA involves symmetrical polyarthritis, typically starting in the small joints of the hands and feet before progressing to larger joints. Patients frequently experience prolonged morning stiffness, joint swelling, and significant pain that impacts physical function. Mechanistically, this disease is driven by a complex interplay of immune cells, including Th17 cells and activated synovial fibroblasts. These cells secrete potent proinflammatory cytokines, most notably TNF-alpha, IL-1, and IL-6. Persistent inflammation would eventually leads to destruction of both cartilage and underlying bone.
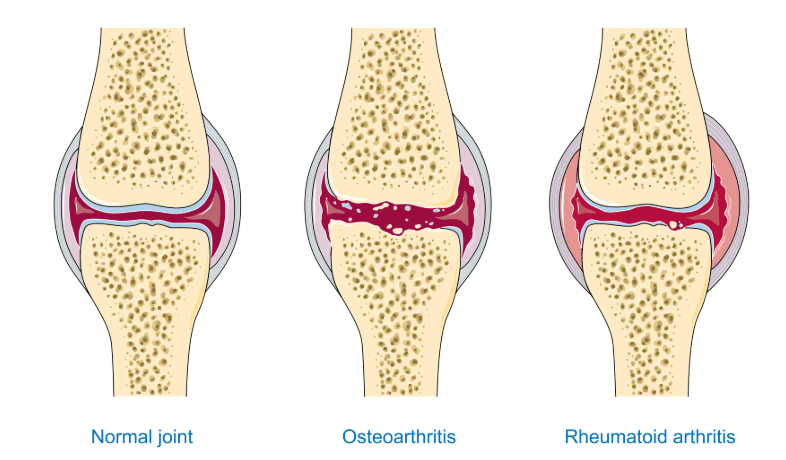
Image credit to Wikimedia commons
Rheumatoid factor (RF) represents one of the earliest identified biomarkers for RA, functioning as an autoantibody directed against the Fc portion of immunoglobulin G (IgG). While RF can be detected in other autoimmune conditions and chronic infections, its high titer is strongly associated with more severe, aggressive disease progression in RA patients. The formation of RF-IgG immune complexes triggers the complement cascade, facilitating local tissue damage and sustained inflammatory responses within the joint space. Anti-Citrullinated Protein Antibodies (ACPAs) are far more specific for RA than RF and are is crucial in early diagnostics. These antibodies target proteins that have undergone conversion of the amino acid arginine into citrulline, which alters structure of more proteins like vimentin. Detection of high-titer ACPAs serves as a powerful prognostic tool, as these patients typically experience a more rapid rate of joint destruction.
Porphyromonas gingivalis and RA
Porphyromonas gingivalis is a Gram-negative, obligate anaerobic bacterium that resides as a primary pathogen within the subgingival biofilms of the human oral cavity. It is classically associated with the development of chronic periodontitis, an inflammatory condition that destroys the supporting structures of the teeth, including the periodontal ligament and alveolar bone. Beyond the oral cavity, this bacterium exhibits remarkable invasive capabilities, allowing it to translocate into the bloodstream and colonize distal tissues like the joints. Its presence in the gingival crevice sets the stage for systemic dissemination, linking oral health directly to systemic autoimmune triggers.
A critical virulence mechanism of P. gingivalis is the expression of a bacterial enzyme called peptidylarginine deiminase (PAD), which catalyzes the citrullination of bacterial and host proteins. While human cells possess PAD enzymes, the PPAD produced by P. gingivalis is unique because it specifically targets bacterial proteins to evade host detection. When these citrullinated proteins are released during chronic periodontal inflammation, the immune system recognizes them as non-self antigens. This creates a supply of citrullinated peptides that stimulate the production of ACPAs, linking oral infection to systemic autoimmunity.
Molecular mimicry occurs when the immune response generated against the citrullinated antigens of P. gingivalis cross-reacts with structurally similar citrullinated proteins in the human joint. Because both the bacterial PPAD and host PAD enzymes produce citrullinated peptides, the antibodies generated to neutralize the infection may inadvertently recognize synovial proteins like fibrinogen or collagen. This cross-reactivity means that even after the initial bacterial trigger is contained, the autoimmune process persists as the immune system targets the joints. The similarity between the bacterial epitopes and the endogenous synovial targets keeps the T and B cell responses active indefinitely. Consequently, the inflammatory milieu of the joint is constantly restimulated, leading to the self-perpetuating nature of chronic RA.
Clinical and Therapeutic Implications
Extensive epidemiological evidence supports a bidirectional association between periodontitis and RA, if patients have one disease they both show higher prevalences of the other. Individuals with severe periodontitis have a significantly elevated risk of developing RA, and conversely, patients with established RA often present with more severe periodontal bone loss. This suggests that the chronic inflammation and bacterial load in the oral cavity may act as a catalyst for systemic disease development. Early diagnosis and treatment of gum disease might reduce the antigenic burden, thereby lowering the probability of systemic autoantibody formation. Integrating dental health into the management of RA represents a promising, though still evolving, paradigm for comprehensive patient care.
Current therapeutic approaches for RA often involve the use of biologics, which are proteins designed to target specific components of the inflammatory cascade. An example is the use of TNF-alpha inhibitors which could neutralize the cytokine responsible for inflammation and tissue destruction. By blocking TNF-alpha activity, the signaling pathway that leads to synovial fibroblast activation and osteoclast recruitment is blocked. Other therapies include B-cell depletion strategies which reduce the production of pathogenic autoantibodies like RF and ACPAs. While these treatments are highly effective at managing symptoms and halting progression, they do not cure the root, which is autoimmune predisposition.
